- ›
- Stories
- ›
- Parkinson’s Disease
- ›
- Parkinson’s Disease: Forced Exercise a Vital Treatment Option
Stories
Parkinson’s Disease: Forced Exercise a Vital Treatment Option

Parkinson’s disease is, by far, one of the most common age-related neurodegenerative disorders in the world. A person is diagnosed with Parkinson’s every nine minutes. In the United States alone, “Nearly one million will be living with Parkinson’s disease (PD) in the U.S. by 2020,” according to Parkinson.org. And there are “More than 10 million people worldwide are living with” symptoms related to Parkinson’s disease.
Over 60,000 people are diagnosed with PD each year. Parkinson’s News Today reports that “The prevalence of the disease ranges from 41 people per 100,000 in the fourth decade of life to more than 1,900 people per 100,000 among those who are 80 and older.”
This disease will dramatically impact someone’s ability to live the full and active lifestyle they want. The symptoms can be hard to treat and differ from case-to-case. In general, though, the most common Parkinson’s symptoms include:
- Tremors that occur when the patient is at rest
- General stiffness
- Slowed and fatigued movement (known as bradykinesia)
- A stooped posture
- Walking and balance difficulties
- Limited facial expressions
- Sudden muscle freezing
- Gastrointestinal problems
- Mood disorders (i.e., depression and anxiety) and cognitive impairments
- Problems sleeping
Parkinson’s symptoms can be both motor and non-motor, and their effect on someone’s quality of life can be crippling. However, just because you or someone you know has been diagnosed with PD doesn’t mean that they can’t live their lives to the fullest. Yes, PD symptoms are challenging, but there are a variety of treatments that help patients manage their symptoms and reclaim their way of life.
If you’re facing a recent diagnosis, or have already been living with Parkinson’s, then this guide is for you. We know how challenging life with PD can be, and we want to help you live a productive and fulfilling life. While various medications can help control the symptoms, when it comes to the only treatment to slow the progression of Parkinson’s, the answer is exercise.
If your symptoms make it difficult to exercise, then the Theracycle motorized exercise bike can help you. The Theracycle enables people to experience improvements in their mobility, stamina, and overall quality of life. This thorough guide will walk you through the ways that forced exercise can be one of the most valuable Parkinson’s treatment options available to you.
Table of Contents:
- Living with Parkinson’s Disease
- Parkinson’s Disease Treatment Options
- Parkinson’s Medications
- Lifestyle Changes
- Exercise and Parkinson’s
- What is Forced Exercise?
- How Can Forced Exercise Relieve Your Parkinson’s Symptoms?
- Reclaim Your Way of Life!
Living with Parkinson’s Disease

Living with Parkinson’s can be difficult. There isn’t currently a cure for PD, and by the time you’re officially diagnosed, your symptoms may already be inhibiting your quality of life.
A 2018 study says that “The progressive death of dopaminergic neurons in the substantia nigra is…one of the main physiological mechanisms manifested before PD, directly interfering with motor behavior.” Of course, PD symptoms aren’t strictly physical, but often involve “cognitive, autonomic, and mood impairments” as well.
Dealing with physical and cognitive impairments may feel overwhelming; even scary. By educating yourself and your care provider, symptom management plans can be put in place to ensure the best quality of life at each stage of the disease.
In fact, with the right support and treatments, you can retain your agency and mobility for years to come. According to the American Parkinson’s Disease Association, living with Parkinson’s usually involves the following lifestyle changes:
- Learning to manage your symptoms and understanding what impacts them
- Incorporating regular exercise and clean eating into your daily routine
- Taking prescribed medications on time, consistently
- Building a strong partnership with your healthcare team
- Participating in clinical trials
- Getting invested in local support groups
Parkinson’s Disease Treatment Options
There are plenty of ways to help improve the way you live with your Parkinson’s symptoms. But with everyone’s symptoms presenting differently, there isn’t a one-size-fits-all treatment guaranteed to work for you and yours. That doesn’t mean there aren’t treatments, medical and otherwise, that will help you live better. To help you get familiar with your options, let’s take a look at the different types of Parkinson’s disease treatments.
Parkinson’s Medications
Your Parkinson’s disease treatment can look a multiple of ways, and each approach has its pros and cons. When it comes to the most commonly used Parkinson’s medications, however, these are the ones that tend to be prescribed the most:
- Carbidopa-levodopa: According to an article on Michigan Health, “the most effective and well-tolerated drug the medical profession has to offer at this time is carbidopa-levodopa.” Upon reaching the brain, this drug becomes synthesized into dopamine. And since PD often attacks the substantia nigra—neurons in the brain responsible for producing dopamine—this medication remains the most popular first-line drug for Parkinson’s patients.
- Dopamine agonists: Parkinson’s News Todays says that dopamine agonists “mimic the effects of dopamine in the brain,” which helps to stave off symptoms. While not regarded to be as effective a treatment as carbidopa-levodopa, it does tend to last longer and can help level out any fluctuations in both medications’ efficiency.
- MAO-B inhibitors: These medications are not as effective as the prior two treatments, but can be valuable for people in the early stages of PD. There are several formulations of MAO-B inhibitors, but most of them involve selegiline and rasagiline and work to slow “the breakdown of levodopa and dopamine in the brain, and may boost the effect of levodopa.”
In addition to these traditional medications, some Parkinson’s patients can undergo deep brain stimulation (DBS) surgery to deal with their symptoms. This isn’t exceedingly common and is used as an alternative only if a patient has stopped responding to their medication.
Parkinson’s News Today defines DBS as “a non-destructive surgical treatment for Parkinson’s disease that involves implanting a device to stimulate targeted regions of the brain with electrical impulses generated by a battery-operated neurostimulator.” This surgery is meant to interrupt the abnormal signal patterns in the patient’s brain that cause motor control issues.
There may not be a cure for Parkinson’s, but there are multiple Parkinson’s disease treatment options that can help alleviate symptoms. And when your symptoms are more manageable, it’ll be easier for you to reclaim critical areas of your lifestyle.
Lifestyle Changes
For some people, medication comes with troublesome side-effects. Surgeries are not often realistic options either, as many of them can be quite costly. In these cases, there is another approach to Parkinson’s disease treatment that may provide the most tangible results for the patient.
A study published by Exercise and Sport Sciences Reviews explains how “Traditional medical and surgical approaches to managing PD are expensive and associated with a variety of side effects that may further compromise” quality of life. However, an exercise routine can improve not only motor and non-motor functions but also your overall mood.
Another study—this one from Clinical Practice & Epidemiology in Mental Health—suggests “that the drugs available for treatment only provide relief of the symptoms, and do not stop the progression of the disease. Therefore, searching for non-pharmacological treatments to help patients is valid and necessary to bring effective treatment to them.”
This doesn't mean that medication isn't essential, but rather, suggests that a well-rounded treatment plan is needed to improve someone’s quality of life. Some drug-free, complementary Parkinson’s disease treatment options, as listed by Parkinson.org include:
- Antioxidants like Vitamins C and E “that fight free radicals and may protect brain cells.”
- A Mediterranean diet that’s “high in monounsaturated fats, such as olive oil, may be beneficial in reducing blood pressure and cardiovascular disease.” This diet often emphasizes fish and salmon, especially those with high amounts of Omega-3 fatty acids.
- Consuming calcium via calcium-fortified-rice and soy milk alternatives to cereal, smoothies, and cooked dishes.
- Other vitamins, supplements, and food options.
Exercise and Parkinson’s
As helpful as medications, lifestyle changes, and natural supplements can be for your Parkinson’s disease treatment regimen, the simple truth is that there are few treatments as universally accepted and encouraged as regular exercise.
Exercise has long been considered one of the most effective forms of Parkinson’s treatment, as it comes with many symptom-relieving benefits without any of the side-effects or price tags often associated with medication and surgery. Parkinsons.org says that “On a daily basis, people with PD who exercise can move more normally than those who do not. We believe that exercise may be contributing to neuroplasticity — helping the brain maintain old connections, form new ones and restore lost ones.”
However, people living with Parkinson’s deal with physical symptoms on an everyday basis. These symptoms can make it difficult to maintain an exercise routine with any regularity, as their ability to exert themselves physically can vary dramatically. This is where forced exercise offers a solution.
What is Forced Exercise?
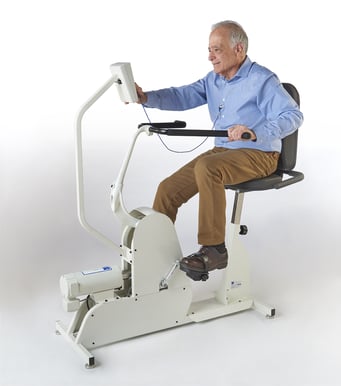 Forced exercise is an exercise regimen that uses an external source—like a motor in an exercise bike—to help someone exert themselves longer, and at higher intensities than they would be able to do on their own. While tandem bicycles can help Parkinson’s patients experience the benefits of forced exercise, riding a tandem bike is not usually an option for them either.
Forced exercise is an exercise regimen that uses an external source—like a motor in an exercise bike—to help someone exert themselves longer, and at higher intensities than they would be able to do on their own. While tandem bicycles can help Parkinson’s patients experience the benefits of forced exercise, riding a tandem bike is not usually an option for them either.
What people need is a motorized exercise bike. The Theracycle allows Parkinson’s patients to exercise regularly without worrying about their physical limitations. Thanks to the Theracycle’s unique motor, every user can get the exercise they need to live healthier lives—regardless of their strength or endurance.
How Can Forced Exercise Relieve Your Parkinson’s Symptoms?
In an article on U.S. News, Dr. Dean Sutherland—a neurologist and Parkinson’s disease specialist—explains how “Exercise releases dopamine into the same parts of the brain that are stimulated by taking medication. That helps with motor issues like stiffness, tremors and muscle freezing.”
Forced exercise not only releases more dopamine into the brain of the user—helping alleviate motor issues and symptoms—but will also keep their body healthy and able. Several studies support this fact, such as a 2009 study conducted by the Cleveland Clinic.
In this study, participants “with mild to moderate idiopathic Parkinson’s” were divided into two separate groups. One group partook in an eight-week forced exercise program—“in which patients’ bodies move beyond the extent they can do so themselves”—while the other group spent the same eight-weeks engaging in “voluntary exercise on a stationary single bicycle.”
At the end of this study, both groups showed improved aerobic fitness. However, the Unified Parkinson’s Disease Rating Scale (UPDRS) motor scores for the users who partook in the forced exercise (FE) regimen improved by 35%. Meanwhile, the other group of patients exhibited no such improvement. Additionally, the “Improvements in clinical measures of rigidity and bradykinesia and biomechanical measures of bimanual dexterity” the forced exercise group experienced “were maintained 4 weeks after FE cessation.”
There is not a single, one-size-fits-all solution to your Parkinson’s disease symptoms. But when it comes to the question “what is the best treatment for Parkinson disease?” there are few solutions as reliable as forced exercise. If you're looking for a Parkinson’s disease treatment that will help you better control your symptoms, then look into how a forced exercise bike can help you.
Reclaim Your Way of Life!

Living with Parkinson’s is no easy thing. The symptoms can make you feel isolated, limited, and can dramatically inhibit your mood and overall way of life if not addressed. While there are plenty of potential Parkinson’s treatment options to mask your symptoms, there are none that can slow the progression of the disease except exercise.
Exercise and Parkinson’s have a long and positive relationship. A study from the FDA even says that people with Parkinson’s who exercise experience “improved sleep, cognitive function, mood, and motor symptoms. One participant stated, ‘exercise is more important than the pills we take.’ A few participants expressed the importance of targeted workouts, including one participant who said, ‘when I am doing a legs workout, I feel the difference in my body.’”
This is why we created the Theracycle motorized stationary bike. With the Theracycle in your home, you can enjoy a Parkinson’s disease treatment that reduces your symptoms’ impact, improving your quality of life. It can bring some independence back, which positively impacts your care provider, too. If you want to learn more about how the Theracycle can help you reclaim the life you want, reach out to us at 1.800.367.6712, or visit our website www.theracycle.com!